Reflecting on how neighbourhood health has evolved from ambition to delivery.
Neighbourhood health is now central to the future of the NHS. As ambition turns into delivery, a more challenging question remains – who is shaping direction and how close to neighbourhoods does that power sit?
This article brings together insight developed over time, reflecting how the NHS has moved from early ambition in 2025 to scaled delivery in 2026, and why the way neighbourhood health is driven matters as much as the model itself.
In 2025, we said
In 2025, neighbourhood health was emerging rather than established. Integrated Care Systems were still forming, and systems were testing how far responsibility could move closer to communities without increasing risk or fragmentation.
Our insight paper, From central oversight to local ambition – redefining roles across the NHS, explored how governance, finance, workforce and neighbourhood care would need to realign if place-based models were to succeed. At its core was a simple proposition – neighbourhood health would only work if systems enabled local leadership rather than tightly managing delivery.
What has changed since
Since then, the policy and operating environment has shifted. Neighbourhood health is now a national delivery priority. Multi-year planning has replaced short-term cycles, Integrated Care Boards operate primarily as strategic commissioners, and neighbourhood health plans and teams are scaling across systems.
Roles are clearer. Expectations are firmer. Pressure is higher. The risk is no longer indecision – it is defaulting to control in the name of pace.
What still holds true
Despite greater clarity, the tension identified in 2025 remains. Neighbourhood health succeeds when systems create space for local judgement, delivery is shaped around relationships and context, and neighbourhoods influence priorities rather than simply absorb them.
It struggles when accountability is confused with control, variation is treated as failure rather than learning, and neighbourhoods carry responsibility without authority. National outcomes, assurance and financial discipline remain critical, but are most effective when exercised through enablement rather than specification.
From national direction to neighbourhood delivery
As systems scale their plans, a more difficult question remains – who is driving neighbourhood health, and how close to neighbourhoods does that direction sit?
Neighbourhood health is shaped by interaction across three levels. National bodies set direction and outcomes. Systems translate these into strategy, assurance and resource decisions. Neighbourhoods bring delivery to life through relationships, leadership and local knowledge.
These levels are interdependent, but their roles are distinct. Neighbourhood health works best when each level focuses on its purpose without drifting into another’s. National requirements provide clarity and consistency. System leadership balances enablement with accountability. Neighbourhood teams shape delivery in response to context, need and trust.
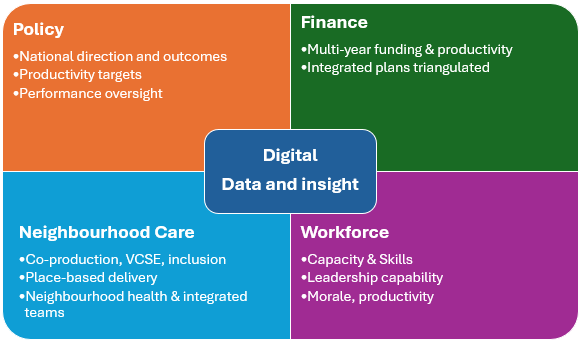
Enablers such as data, digital capability, workforce and shared insight support these relationships when they strengthen learning and understanding across levels. They are most effective when they reinforce local judgement rather than replace it.
When these roles remain in balance, neighbourhood health is driven through enablement rather than control, and variation can be understood as learning rather than failure.
The Hub’s role
The Hub supports systems, places and neighbourhoods to navigate this terrain with confidence. We do not offer a single model or solution. We help partners make sense of shifting roles, surface assumptions early, and protect the conditions that allow neighbourhood health to succeed in practice.
If you are grappling with how neighbourhood health is being driven in your system, you are not alone – and you are welcome to continue the conversation with us by getting in touch: [email protected]
